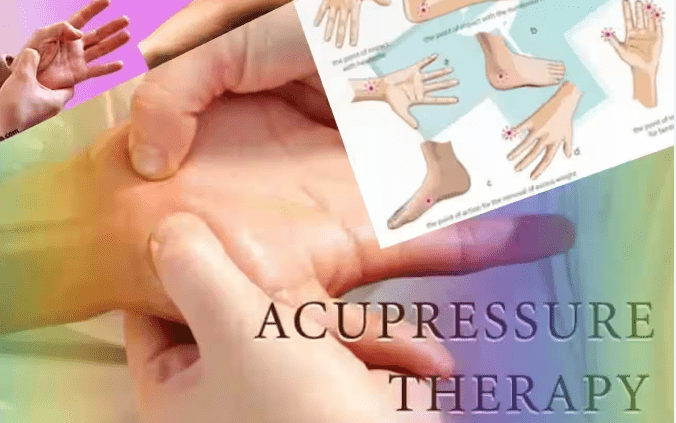
Discover the Benefits of Self-Healing Acupressure Therapy – Improve Your Health and Wellbeing
Welcome to the world of Acupressure Therapy – a time-tested, natural way of staying fit and healthy from within. If…

Welcome to the world of Acupressure Therapy – a time-tested, natural way of staying fit and healthy from within. If…
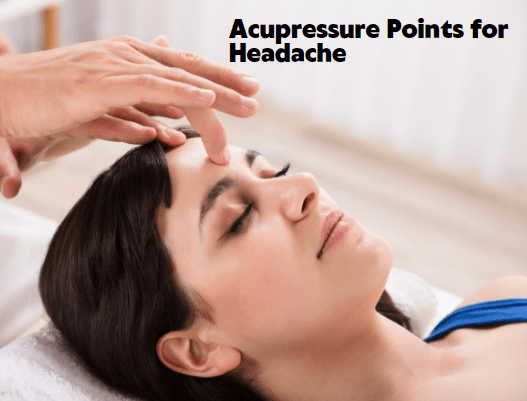
Acupressure, an ancient practice of traditional Chinese medicine, may seem enigmatic due to its reliance on invisible pressure points and…

Acupressure, a type of alternative medicine similar to acupuncture, aims to stimulate pressure points along the meridian lines of the…

Yoga for Hair Growth– For generations, gorgeous hair has been associated with glamour, femininity, and self-confidence. However, with changing lifestyles…

Stress is an inevitable part of life. However, those suffering from a combination of stress and depression may experience more…

Acupuncture vs Acupressure: Acupuncture and acupressure are both alternative therapies for pain relief, but what’s the difference? Discover how these…

9 Acupressure Points for Insomnia: It’s well-known that getting a good night’s sleep is essential for our overall health and…

How many hours of Sleep: The amount of sleep you require changes throughout your life and depends on the number…

Best Acupressure points for back pain– Back pain is a common problem faced by many people, especially those who sit…

Learn our quick and chemical-free ways How to clean your yoga mat so it will look and smell fresh Here…

Bloom Nutrition Review is a comprehensive and informative publication that delves into the latest advancements and trends in the field…